While many women choose to wait until they’ve finished having children and breastfeeding before having a reduction, for others, this isn’t an option.
Other women may not have met someone they would like to have children with and wonder if they ever will. They don’t want to put off having their breast reduction for a scenario that may or may not eventuate.
Some women have a breast reduction without considering the impact it will have on future breastfeeding. For others, it just feels too abstract and irrelevant for where they are in their life at the time of surgery.
No doubt, you have your own story about why you want to have breast reduction and whether you want to breastfeed in the future.
I think it is important for women to make informed choices about their bodies that will support their wishes now but also in the long-term.
Right now, a baby may be the furthest thing from your mind, especially if you’re really young. However, I want you to have the knowledge you need to make an empowered decision that suits where you are now in your life, and that keeps your options open.
Why Breastfeeding is Important
I am a big advocate for breastfeeding; I breastfed for about five years in total. Breastfeeding was important to me, and I didn’t want to risk my ability to breastfeed by having my breast reduction surgery until after I’d finished having children.
That said, I don’t believe breastfeeding is always best when a mother and baby are not thriving. There are situations where breastfeeding needs to be supplemented or abandoned altogether. At the end of the day, the most important thing is the well-being of the mother and child.

There are a number of advantages to breastfeeding for both
the baby and mother
“It is also important to remember that nursing is so much more than nutrition. By breastfeeding our babies, we meet a whole range of emotional needs as well. When we understand success in this way, we are aware of the power we have to make breastfeeding possible and to be wholly satisfied with whatever unique direction our breastfeeding relationship may take. It is this empowerment that gives us strength in vulnerable moments and keeps the knowledge uppermost in our minds that we alone determine what success will mean for us.”
~Diana West
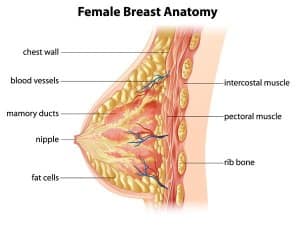
The type of surgery you have, along with any complications, will have a big impact on whether breastfeeding post-reduction is possible.
If you have a free nipple graft (FNG), you will not be able to breastfeed because it involves totally removing the nipple and areola. This is why a free nipple graft should be avoided if possible if you want to breastfeed. If for some reason, this is the only option available to you, you really want to breastfeed in the future, you may consider postponing your surgery until you have had children.
While a liposuction-only reduction does not normally affect breastfeeding, it only removes a limited amount of breast tissue and does not provide any lift to the breasts.
Pedicle surgical methods, such as the Vertical/Anchor or the Inverted-T/Lollipop, give you a high chance of breastfeeding because the areola and nipple function are normally maintained.
It is important to note that if you have your areola resized, there is a greater risk of damaging the nerves that are part of the letdown reflex (this is the reflex that tells your body to release milk).
The letdown reflex is important because it allows milk to be produced and stored in your breasts, ready for when your baby needs to feed. If your letdown reflex is affected or doesn’t occur, less milk gets removed from your breasts which can then impact your milk supply.
If you let your surgeon know you want to breastfeed when you have children, they can make sure enough of the areola complex remains in order to maximize your ability to breastfeed in the future.
There are no guarantees that just because you have a pedicle type of breast reduction, that you will be able to breastfeed. The truth is, you won’t know until you’re holding your sweet baby in your arms.
How Breastfeeding Affect Breast Size
Many women experience a change in the breasts during pregnancy as their body prepares for breastfeeding. Breasts will get bigger during pregnancy and may return to the size they were before you had surgery. This can be a scary prospect for many women, however, keep in mind that pregnancy increases breast size, not lactation. With or without surgery, your breasts are likely to increase during pregnancy. After the birth of your baby and the first few weeks of breastfeeding, your breasts should return to their pre-pregnancy size. If your breasts enlarge a lot during pregnancy, you may find you have more stretch marks afterwards.
Maximizing Milk Supply
Some women, whether they have had a breast reduction or not, experience milk supply issues. Women who have had a breast reduction often have a higher chance of having low milk supply. However, this doesn’t mean you can’t breastfeed. There are things you can do to try and increase your supply. And if necessary, you supplement breastfeeding with formula.
Things that affect milk supply include stress, medications, positioning and attachment of the baby to the breast, diet and hydration.
Define Your Own Success
We live in a world of constant judgment. As a new mother, you will undoubtedly receive advice from people with good intentions who only want what is best for you and your baby. Their advice will depend on their view of the world. Some will tell you to give up on breastfeeding because it’s too hard, especially if you have supply issues. Others may tell you your baby needs breast milk or they will be scarred for life. Breast reduction surgery often brings out a lot of judgment as well!
As women, we need to define our own success. If breastfeeding is important to you, then do it in whatever way works best for you.
Here’s a quote from the book, Defining Your Own Success: Breastfeeding After Breast Reduction Surgery by Diana West:
“Among women who have had breast reduction surgery and are now breastfeeding, it is often said that "We each define our own success." As it is used here, "success" is not an absolute term referring to a continuum of less to more milk produced. Rather, it is defined by the degree of satisfaction each woman and her baby derive from the breastfeeding relationship they create together. It is not determined by the amount of milk a woman produces. Each woman's experience of success will be different; some may be able to breastfeed exclusively, while others may need to supplement the baby's entire nutritional requirement."
My wish for you, and all mothers, is that you do what is right for you and your baby, and that you get the support you need.
Get More Information
Breastfeeding after a reduction is a big topic. To explore this issue more, you may like to check out these books:
- Defining Your Own Success: Breastfeeding after Breast Reduction Surgery by Diana West
- Breastfeeding after Breast and Nipple Procedures by Diana West and Elliot Hirsch
- The Breastfeeding Mother’s Guide to Making More Milk by Diana West and Lisa Marasco
For more information on these books and on breastfeeding after a reduction, you may like to visit the Breastfeeding After Reduction website: www.bfar.org


Read All the Breast Reduction Surgery Blogs
In this special series of blog posts, Ayesha Hilton shares with you:
The Risks & Benefits of Breast Reduction Surgery
The main types of Breast Reduction Techniques
Breast feeding after a Breast Reduction
How to find a surgeon

Get Your Copy of
Breast Reduction Surgery
The Complete Guide to Breast Reduction Surgery & Recovery